ASMI and Its Effective Treatment for Back Pain
Injuring Your Back Over Time
As the spine’s flexibility and mobility of youth fades, the lower back and neck become increasingly overworked and over stressed. This often leads to herniated discs (following even minor injury) or chronic back pain and sciatica. Research has shown that increasing spinal flexibility and mobility restores function and helps to relieve pain.
Current Treatments for Back Pain
Today most treatment for back pain includes pain relievers, injections, physical therapy, chiropractic or surgery. If you are a person who has had these done with only mild to moderate results at best then there is another revolutionary option recently approved by the FDA.
Today, with the use of the Advanced Spinal Mobilization Instrument (ASMI), trained practitioners can perform an effective and lasting treatment for patients with back pain. Through the gentle, passive movement of pairs of spinal vertebrae and the stimulation of the surrounding spinal muscles and reflexes, we can return flexibility and mobility, restoring function and relieving pain.
The Advanced Spinal Mobilizer Instrument
One of the most effective means to restore flexibility and mobility to the spine is the technique of Spinal Mobilization. The strength, consistency, repetition required however to effectively treat patients is beyond the abilities of most practitioners and so the Advanced Spinal Mobilization Instrument was developed.
Cleared by the United States Food and Drug Administration (FDA) in 2005, the ASMI is indicated for use and designed as an extension of the practitioner’s own hands, combining precise and infinitely variable control.
Developed in the United Kingdom there are currently only three clinics in the United States that have this unique hand held device.
The patented handset incorporates four moving pads powered by variably controllable electro-pneumatics. Each treatment is delivered in three modes, an introductory or “spasm” mode, a para-spinal muscle “reflex” stimulation mode and the “mobilization” mode. Each mode is used to varying degrees depending on the patient’s condition as determined by the practitioner.
The ASMI is used to gently rock neighboring vertebrae back and forth. The condition of the joint determines the response to the applied effort. Initially the joint may be fixed or move imperceptibly. With time and successive treatments, flexibility, mobility and function is restored to the back and spine.
ASMI is Truly a Unique Treatment for Back Pain
Treatments are performed with patients lying prone or face down on a specially-designed treatment table that places the patient in a comfortable position while providing gentle passive traction opening up the joints in the spine.
As the instrument is worked up and down the spine, each vertebra is gently counter-rotated with its neighbors. In many cases, after only a few treatment sessions, pain is progressively relieved!
- The introductory or Spasm mode always begins and ends a treatment, relaxing the patient.
- In the Reflex mode, short taps are applied to and stimulate and “wake up” para-spinal muscle groups.
- In the Mobilization mode, gentle, moderate or firm hands-on treatment is applied to pairs of adjacent vertebrae producing counter-rotational movement and spinal mobilization.
Back pain accounts for over $90 billion a year in health care costs in the United States alone! With the introduction of the Advanced Spinal Mobilization Instrument (ASMI), there is a safe, efficacious, drug free, surgery free, non-invasive and conservative alternative to treat the millions of back pain sufferers in the United States and around the world.
Diabetes and The Role of Physical Therapy
Physical Therapy is a Valuable Treatment for Diabetes
Physical therapy can be very valuable in the treatment of diabetes. Many people do not know how to exercise properly and safely. A physical therapist is specially trained to utilize the best exercise for each person’s condition, as well as teach which exercises should not be used.
Some individuals or personal trainers may not be as knowledgeable about the precautions for various medical conditions. Proper positioning of the body while performing an exercise is important to optimize the benefits of the exercise.
Benefits of Exercise:
- Improve glucose levels (especially for those with type-2 diabetes)
- Decrease use of oral hypoglycemic agents
- Reduce body fat
- Improve the cardiovascular system
- Promote stress reduction
- Increase function and strength
- Improve balance and decrease fall risk
- Reduce blood pressure
- Improve carbohydrate metabolism
- Improve well-being and diabetes control
Physical Therapy Evaluation
Each person referred for physical therapy receives a personal evaluation by a licensed physical therapist. Components of the evaluation include a thorough medical history, examination of co-mobidities, and questions about glycemic (blood sugar) control.
Each person should discuss physical therapy and exercise goals with the physical therapist, including any functional problems or difficulties. The physcial therapist will assess the patient’s strength, range of motion, flexibility, gait, balance, sensation, posture, joint mobility, and soft tissue tightness. An examination of the skin with an emphasis on the legs will also be performed.
Physical Therapy Treatment
The results of the physical therapy evaluation are used to formulate a treatment plan. The plan may include joint mobilization, soft tissue mobilization, range of motion exercises, gait training, balance activities, strengthening exercises, and different types of aerobic exercises.
Since there are many different problems associated with diabetes, each person’s plan of treatment may vary. People with cardiovascular or heart problems may need a treadmill test and evaluation by a cardiologist before beginning an exercise program. This is especially important if the person has been sedentary and has had diabetes for a long period of time.
Peripheral arterial disease, which is another manifestation of diabetes, is very responsive to the correct physical therapy plan of treatment. People with peripheral arterial disease (especially those with intermittent claudication) can make significant gains with therapy, decreasing leg pain while increasing walking distance.
People with retinopathy should avoid anaerobic exercise and should not perform any jarring or straining maneuvers. For people with nephropathy (kidney disease), low-moderate exercise may be performed, refraining from high-intensity or strenuous exercises.
People with peripheral neuropathy may benefit from exercise, but the exercises must be specifically tailored to their problems due to the dangers associated with the loss of protective sensation in the feet. Intense weight bearing exercise should be avoided since this could possibly lead to ulcerations or fractures.
Exercise Precautions
Before and after exercising, individuals should check his or her feet for blisters or reddened areas of skin. Blood glucose should be measured before exercise and if greater than 250mg/dl, exercise should not be performed.
Carbohydrates should be taken every hour during exercise if the blood sugar is 80 – 100mg/dl. Post-exercise blood glucose levels should also be measured, since exercise usually decreases the amount of glucose in the blood. Good glycemic control is necessary while exercising.
Before deciding if exercise should even be performed, a physician and physical therapist must first determine any contraindications to exercise. It is essential for each person to be medically stable before beginning any exercise program. Safety is of the utmost importance.
Safety issues should be discussed with the physical therapist prior to exercising for a thorough understanding of precautions.
Results
Physical therapy is a powerful adjunct to medical treatment. A life-style of exercise for people with diabetes can greatly help to maintain blood sugar levels, increase strength, reduce the risk of cardiovascular disease, and increase functional ability.
Talk to your doctor about the possibility of including physical therapy in your diabetes treatment plan. The sooner your start, the sooner you will be on your way to a healthier life!
Need Help Managing Your Diabetes?
If you or a loved one suffers with diabetes and would like some help controlling your diabetes, contact us at one of our 7 locations: Click Here to find a location near you.
Trigger Point Dry Needling
What is Trigger Point Dry Needling? And Can It Help Me?
Yes, in recent studies, combining dry needling techniques with other manual and rehabilitative methods has shown to be very effective in the treatment of chronic pain and reducing recovery time.
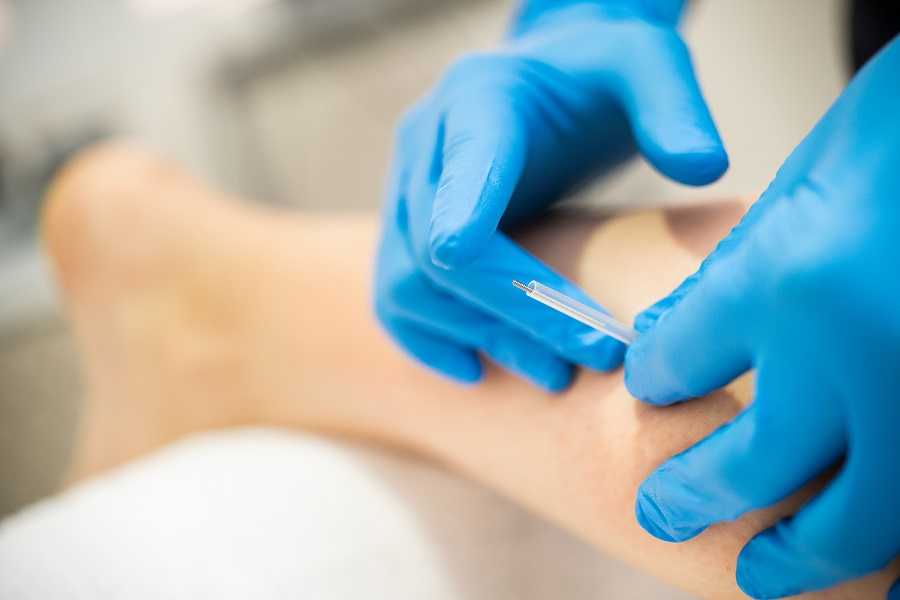
According to multiple physical therapy state boards, Trigger Point Dry Needling (Dry Needling) or Intramuscular Manual Therapy is “a skilled intervention performed by a physical therapist using a thin filiform needle to penetrate the skin and stimulate underlying neural, muscular, and connective tissues for the evaluation and management of neuro-musculoskeletal pain and movement impairments.”
In other words, it is a form of treatment where a physical therapist uses thin ‘dry’ needles pressed through the skin to stimulate a trigger point and thereby help relieve pain caused by muscular tightness and spasms, increase motion and improve our patients’ function.
How Does Trigger Point Dry Needling Work?
A number of theories exist as to how Dry Needling works. The theories that we agree on at Coppola Physical therapy is that dry needling works by disrupting a reflex arc of contracted tissue as well as stimulating biochemical changes to allow improved blood flow and healing to the area.
Another theory held by the Journal of Orthopedics and Sports Physical Therapy “dry needling may release the tight muscle bands associated with trigger points and lead to decreased pain and improved function.”
How Is Dry Needling Performed?
A physical therapist utilizes a very thin filament needle (acupuncture needle). While the physical therapist uses an acupuncture needle the treatment is not considered acupuncture. Dry needling is based on Western physiologic approaches.
According to James Dunning…. Unlike acupuncture, dry needling “does not attempt to move qi (chi) along a meridian, nor does it rely on diagnosis from traditional Chinese acupuncture or Oriental medicine.”
The needle is pressed or inserted into the trigger point and a local twitch response is ideally elicited. This twitch response is an involuntary contraction of the muscle that allows the muscle to relax. Sometimes electrical stimulation is applied to the needle to elicit these twitches to help the muscle relax as well.
What Are Trigger Points?
Trigger points are hyper-irritable contractions or knots found in tight bands of muscles. And according to the American Family Physician trigger points are “discrete, focal, hyper-irritable spots located in a taut band of skeletal muscle. They produce pain locally and in a referred pattern and often accompany chronic musculoskeletal disorders.”
A patient will present with pain when adding pressure to a taut band which ‘triggers’ a referral of symptoms spread beyond the muscle and often times away from the actual trigger point. Trigger points can affect the local area of pain but also can refer to other parts of the body which can all effect strength, flexibility, and coordination of muscles.
How Long Does It Take To Experience Relief With Dry Needling?
After the dry needling treatment, many people note immediate improvement in symptoms of tightness and pain relief. While many patients experience immediate relief, many cases take 24 to 48 hours and this is often accompanied by soreness from the treatment itself.
What Does Dry Needling Feel Like?
When the needle is pressed into the skin some patients don’t report any pain or feelings while others vary in their reaction. Most people report a slight pin prick feeling while others experience a dull ache as the needle penetrates the tissue. Often times a twitch is elicited when the needle penetrates the trigger point. Most of the aching subsides as the needle remains in place for a few moments.
What Conditions Can Be Treated With Dry Needling?
Dry Needling helps to reduce muscle tension and active trigger points in muscles. Conditions that are most often the cause of trigger points include osteoarthritis, muscle strains and ligament sprains, joint injury, and nerve irritation as in the case of herniated discs in the neck or back.
Commonly treated diagnoses include but are not limited to the following:
• Sciatica
• Osteoarthritis
• Neck pain
• Headaches and migraines
• Shoulder pain
• Frozen shoulder
• Knee pain
• Plantar fasciitis
• Hip bursitis
• Hamstring and lower back injuries
• Chronic pain syndromes
• Carpal Tunnel Syndrome
• Lateral Epicondylitis
• Medial Epicondylitis
• Temporo-mandibular joint dysfunction (TMJ)
To learn more about how we can help you or a family member by using Trigger Point Dry Needling, call us at Coppola Physical Therapy and ask for one of our physical therapists trained in trigger point dry needling.
Click on the following link to find a Coppola Physical Therapy location near you: 9 Convenient Locations
What Does The Research Say About Dry Needling?
- Dry needling combined with exercise showed significant improvement in pain, motion, trigger point reduction, and function following a total knee replacement (Nunez-Cortes R et. al)
- There is moderate evidence that dry needling on trigger points can relieve low back pain when coupled with other therapies (Liu L et. al.)
- While additional studies are needed, Kietrys DM et. al. states that “based on the best current available evidence, we recommend dry needling, compared to sham or placebo, for decreasing pain…in patients with upper-quadrant myofascial trigger points (Kietrys DM et. al.)
- A study by Koppenhaver S et. al. found improvement in shoulder motion and reduced pain sensitivity after dry needling of the infraspinatus muscle in patients with subacromial pain syndrome (pain in the shoulder). (Koppenhaver S et. al.)
- It is noted that very low-quality to moderate-quality evidence suggests that dry needling performed by PTs is more effective than no treatment…in patients presenting with musculoskeletal pain at 12-week follow-up (Gattie E, Cleland JA, Snodgrass S)
- In a study by Krey, Borchers, and McCarney the evidence suggests that dry needling to tendons improved outcome measures in patients with tendinopathy. (Krey D, Borchers J, McCarney K)
- France et. al. showed significant improvement in cervicogenic headaches (headaches coming from the neck musculature) following dry needling treatments (France et. al.)
- A double-blinded, placebo-controlled study by Tekin et. al. showed significant decreases in pain, improved quality of life, and decreased need for medicines… (Tekin et. al.)
- Six weeks of dry needling treatment of patients suffering from fibromyalgia noted significant differences in pain, fatigue, outcomes scores, pressure pain threshold, and global subjective improvement in a study by Casanueva et. al. (Casanueva et. al.)
- In a study by the International Journal of General Medicine a PT anesthetized then treated with dry needling, sham treatment, and nothing. The dry needling significantly decreased the need for post-surgical analgesics and had the same degree of pain reduction in one month as the control patients achieved in 6 months. (Intl Journal of General Medicine).
Arthritis and the Role of Physical Therapy
Arthritis is an illness that can cause pain and swelling in your joints. Joints are places where two bones meet, such as your elbow or knee. Some kinds of arthritis can cause problems in other organs, such as your eyes, or in your chest. It can affect your skin, too.
How Can Physical Therapists Help?
Physical therapists can teach you exercises designed to preserve the strength and use of your joints. They can show you the best way to move from one position to another. They can also teach you how to use walking aids such as crutches, a walker, or a cane when needed.
What are the Goals of Treatment?
The therapists on your health care team will work closely with your doctor to tailor a program to your specific needs, whether your arthritic problems are widespread or confined to one joint or body area.
The goals of treatment are to:
- Prevent loss of use of the joints
- Restore abilities that may have been lost
- Help you adapt to new activity levels
- Maintain your fitness
- Maintain your ability to take part in the activities you choose with minimal help from others
Therapy should be started early in order to reduce painful symptoms of inflammation, prevent deformity and permanent joint stiffness, and maintain strength in the surrounding muscles.
When pain and swelling are better controlled, treatment plans may include exercises to increase range of motion, and improve muscle strength and endurance.
What are Some Benefits of Physical Therapy Programs?
Physical therapy programs may provide:
- Education about your kind of arthritis, so that you can be a well-informed member of your health care team,
- Foot care advice, including information on how to choose well-fitting shoes with shock-absorbing outer soles, and sculptured (orthotic) insoles molded exactly to the contour of each foot,
- Therapeutic methods, including physical techniques and activity modifications, to relieve discomfort and improve performance.
Joint Protection Techniques
A therapist can show you ways to do everyday tasks without worsening pain or producing joint damage. Some joint protection techniques include:
- Use proper body mechanics to get in and out of a car, chair or tub, as well as for lifting objects.
- Use your strongest joints and muscles to reduce the stress on smaller joints. For example, carry a purse or briefcase with a shoulder strap rather than in your hand.
- Distribute pressure to minimize stress on any one joint. Lift dishes with both palms rather than with your fingers, and carry heavy loads in your arms instead of with your hands.
- If your hands are affected by arthritis, avoid tight gripping, pinching, squeezing, and twisting. Ways to accomplish the same tasks with alternate methods or tools can usually be found.
Final Thoughts
As the central member of your treatment team, you are the person responsible for following through with your therapy program. This includes taking medicines as prescribed, continuing daily exercises, having a positive attitude, patience and persistence will help you to get the greatest benefit from your physical therapy activities.
You should discuss questions and problems with your doctor and your therapist as they come up so that the program can be adjusted to best meet your needs.
If you are experiencing any pain or issues with arthritis contact your nearest Coppola Physical Therapy. We can be found at: https://www.coppolapt.com/locations